Insulin Resistance and Sensitivity
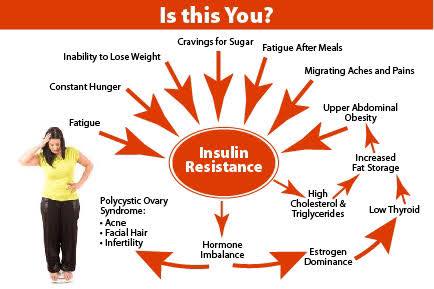
Insulin Resistance and Sensitivity
We hear a lot about insulin resitance and insulin sensitivity in the media these days, but few really understand what insulin is and what these terms mean.
So, we’ll try and explain a little bit here.
Insulin is a hormone that is produced by the pancreas primarily after you eat carbs. Carbs are absorbed into our bloodstream and elevate our blood sugar levels – this is what the pancreas detects and releases insulin to help the body process this glucose.
When we are healthy, the insulin binds with cell receptors, activating other receptors to absorb the glucose from the bloodstream, moving it into cells to be used for energy.
Insulin Resistance and Sensitivity
These are not absolute terms and are more a continuum of physical state. We are able to change the way our cells respond to insulin to become more sensitive.
Resistance occurs when your cells are less affected by insulin and the receptors don’t bind properly. Basically, it is as though there are locks on the doors to your cells, not allowing insulin to enter. When this occurs, your pancreas will secrete more and more insulin due to the continued detection of glucose in the bloodstream. The pancreas will think that more “keys” are needed to open the door to the cells.
High levels of insulin and glucose remain in your body, with neither going anywhere they are meant to. This can result in low energy levels as your cells are not receiving the fuel they need, and will also have other negative and adverse affects on other bodily processes.
Some of these negative effects include fat gain, higher cortisol levels, increased triglyceride levels, leading to atherosclerosis and heart disease, the production of free radicals leading to chronic inflammation and disease.
Simple Tips to improve insulin sensitivity
- Eat a high protein, low carb diet;
- Manage the glycemic response through the intake of fibrous, low-glycemic foods;
- Limit fructose in your diet;
- Engage in strength and interval training programs;
- Be physical on a daily basis & generally more active;
- Ensure your basic nutrients are adequately supported by your diet & supplementation (Our top 5 are:- Multivitamin, Fishoil, Magnesium, Zinc, Vitamin D).
A well-structured eating plan works best when it’s tailored to your body, not copied from a trend floating around the internet. That’s where a qualified dietician steps in. A good professional doesn’t just hand you a chart and send you off—they study your lifestyle, medical history, preferences, and even your daily schedule before shaping a practical plan you can actually stick to. Consistency, after all, has always beaten fads.
If you’re unsure where to begin, consulting a reputable health center can make the process far more reliable and structured. They typically assess your metabolic markers, identify nutritional gaps, and provide guidance that aligns with your long-term health goals rather than quick fixes. With proper monitoring and expert direction, improving insulin sensitivity becomes a steady, manageable journey—not a guessing game.
As individuals begin improving insulin sensitivity through nutrition, exercise, and consistent lifestyle habits, some may also explore medically guided strategies that complement these foundational efforts and support metabolic balance more effectively. Weight regulation and insulin response are closely connected through hormonal signaling, appetite control, and glucose metabolism, which is why healthcare professionals may sometimes introduce targeted treatments when lifestyle measures alone do not fully address metabolic challenges.
One area of growing clinical interest involves medications that act on the glucagon-like peptide-1 (GLP-1) pathway, helping regulate appetite, slow gastric emptying, and support more stable blood sugar control as part of a broader health strategy. Within this developing approach to metabolic care, services associated with Coby Health reflect how medically supervised weight-management treatments can be integrated alongside nutritional guidance, activity planning, and regular health monitoring.
When approached in combination rather than isolation, these elements reinforce the same principle outlined earlier: sustainable improvements in insulin sensitivity and overall wellbeing are most effective when dietary awareness, physical activity, and appropriate medical support work together as part of a structured, long-term health regimen.
Please comment should you have any queries ![]()
T&Cxx
